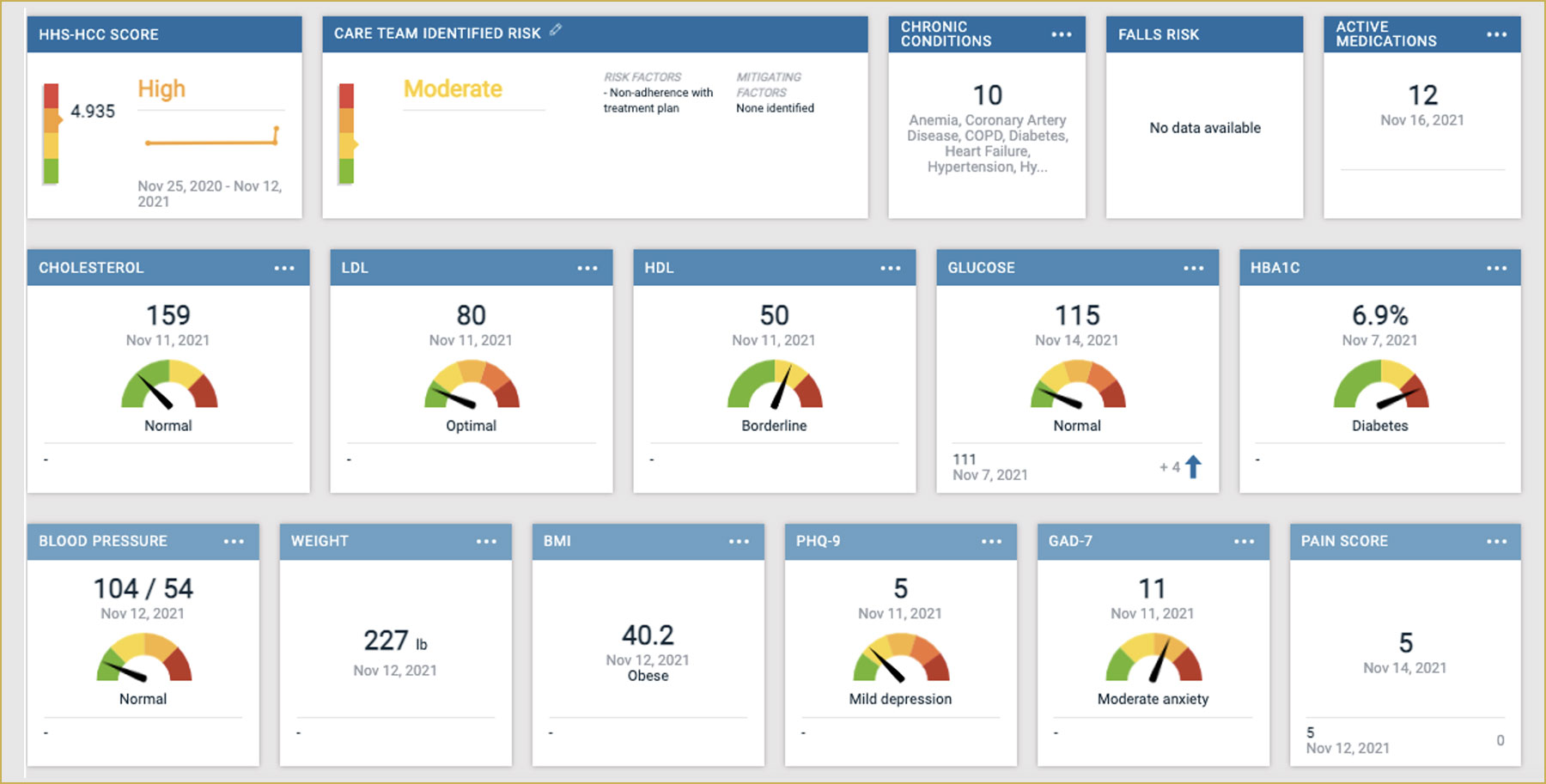
Mitigating Risk Through Actionable Reporting
Privis Health incorporates each stakeholder’s specific quality score cards, satisfaction surveys, Net Promoter Score (NPS), and Risk Adjustment Factor (RAF) score. We report on the metrics that matter most to providers, payors, and organizations, ensuring they move the needle on quality metrics.